Praising the Unexpected: What I’ve Learned from Hospital Admissions
Written by |

Life can change in a blink of the eye. One moment you may be on vacation in Hawaii, and the next you can be on a ventilator being medically evacuated back to the mainland. Being hospitalized unexpectedly is never a happy feeling. Instead, it can bring feelings of guilt, uncertainty, fear, frustration, and sometimes anger. But in the midst of all the negativity, it also can present you with a beautiful outlook of the world.
I’ve had my share of abrupt — some may use the adjective “accidental” — hospitalizations. I’ve gone in through the emergency department at odd hours, and I’ve gone to the clinic confident I would be returning home, only to be told to head to the admissions department. Every human is individual. And, although we all are unique, I can assure you a surprise hospitalization is never welcomed.
Mornings on clinic days often are turbulent. It means waking up earlier than normal, packing morning medications, having an adequate breakfast, doing breathing treatments and chest percussion therapy, and braving the morning traffic — all before arriving to the hospital. These days bring stress, but in the face of all the agony, it permits sharing intimate moments and building bonds with the close relationships I already embrace. The car rides allow for conversation, laughs, and dancing to music. And the breathing treatments allow for open ears as I listen to others speak.
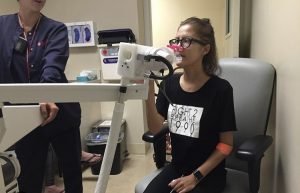
Pulmonary function tests are a range of tests that measure how well the lungs inhale and exhale air and how efficiently they transfer oxygen into the blood.
Upon making it to the hospital, the first task is entering the lab for blood work. Once complete, I walk down the long hall to radiology. When called, I first stand up with my chest against the imaging machine, then turn to the left with my chest against the board for the second view. Afterward I always step into the back area where my family watches me.
I like to think that after 26 years I can read and imagine and, if not, at least notice similarities and differences between my images. My family feels the same and we discuss the X-ray together while listing questions for the visit before seeing the team.
The last responsibility is pulmonary function tests. Once the test begins I am instructed to breathe in two normal breaths, and on the third one I take a deep breath to fill my lungs with the maximum volume allowed, then immediately push all the oxygen out as strong as possible until completely empty. As I do this, my brother, mom, or boyfriend stand by cheering for me and encouraging me to do my absolute best.
Prior to my double-lung transplant I had a lung capacity of 14%, and now I have 56% lung capacity, thanks to my donor and the important caregivers in my life.

People with cystic fibrosis do breathing treatments and chest percussion therapy four times a day, lasting an hour. I often times do my breathing treatments in the car on the way to the hospital to save time.
I sit in the clinic waiting room with my mask, where I am able to meet lots of patients experiencing life in similar ways. It always warms my heart to meet post-transplant people who are succeeding in life and living healthy. It motivates and inspires me.
When my name is called, I do vitals and get comfortable in my examination room. I usually have another snack, do my morning medications, and sneak in sleep whenever possible. Many times my brother and I snuggle up on the examination table, snoring.
We usually can tell when I will be hospitalized, but sometimes the news comes suddenly. Generally it is to protect you, and prevent future problems. The doctors are always looking to future my health as long as possible to add not only quantity of life, but also quality of life. Although I know as a patient my team is looking out for my best interests, hearing the words “we are going to admit you” can be heart-breaking. It can even bring feelings of blame onto myself for not staying healthy longer, and “taking steps backward” in my transplant recovery/survival.
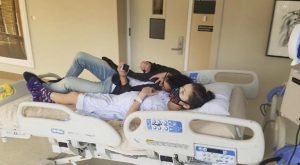
Grateful to the loving people in my life who hold my hand, cheer me on, tell me I can do anything, and even share a hospital bed with me to keep me comfortable, happy, and positive.
While sitting in the admission department waiting, I am frequently making the necessary calls needed to reschedule events, cancel meet-ups, and asking family to alter their plans to visit and support me. I try to stay busy while I wait, all with a loved one by my side.
Being admitted to the hospital leaves a lot of room to grow relationships with the people who come to visit and stay with you. It breaks away from the everyday distractions and forces communication. It can quickly demonstrate who are true friends, and who are friends only when they choose to be during happy and healthy moments.
Unfortunately living with a terminal disease means having numerous phases of illness. However, it is not all negative. It can teach us to be thankful for the beauty of every day outside the four white walls of the hospital.
***
Note: Cystic Fibrosis News Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Cystic Fibrosis News Today, or its parent company, Bionews Services, and are intended to spark discussion about issues pertaining to cystic fibrosis.







Leave a comment
Fill in the required fields to post. Your email address will not be published.