FAQs about cystic fibrosis
According to the Cystic Fibrosis Foundation, there are nearly 40,000 people living with cystic fibrosis in the U.S., and more than 100,000 people living with the disease worldwide. Cystic fibrosis can affect people of every race and ethnic group.
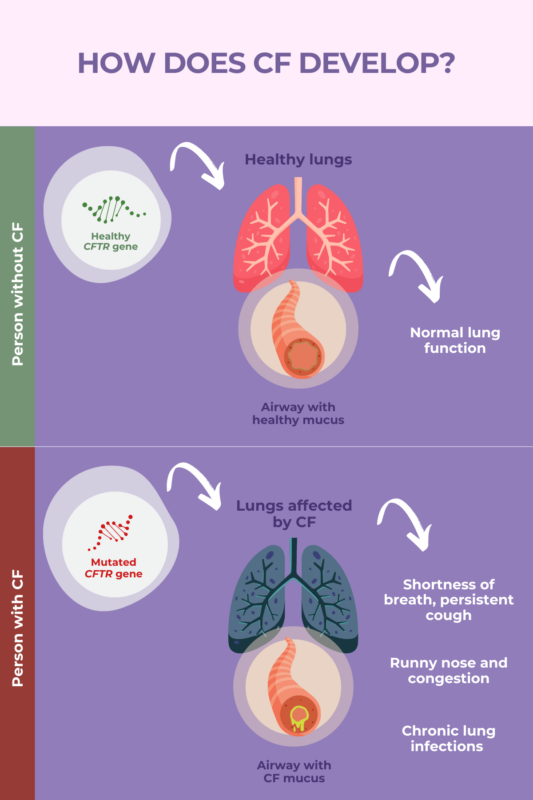
Cystic fibrosis is characterized by the production of abnormally thick, sticky mucus. This mucus builds up in the body’s organs, particularly the lungs and digestive system, and is mainly responsible for driving disease symptoms. The buildup of thick mucus can cause clogs that interfere with organ function, and it sets the stage for infections and inflammation that cause progressive damage over time.
Everyone inherits two copies of the CFTR gene, mutations in which underlie cystic fibrosis (CF), one from each biological parent. CF is inherited in an autosomal recessive manner, which means the disease will only develop if there is a mutation in both copies of this gene.
Cystic fibrosis is a genetic disorder caused by mutations that are inherited from a person’s biological parents. It is not contagious. However, people with CF may be at increased risk from infections, so patients often have to take extra precautions to avoid other diseases that are contagious.
Cystic fibrosis (CF) is a recessive condition, meaning the disease will only develop if an individual carries mutations in both copies of the CFTR gene, one inherited from each biological parent. A person with one mutated copy of the CFTR gene alongside a second healthy copy will not develop CF but may pass the disease-causing mutation on to any biological children. Such individuals are called carriers.
 Fact-checked by
Fact-checked by