I Have Cystic Fibrosis and I Am Traumatized
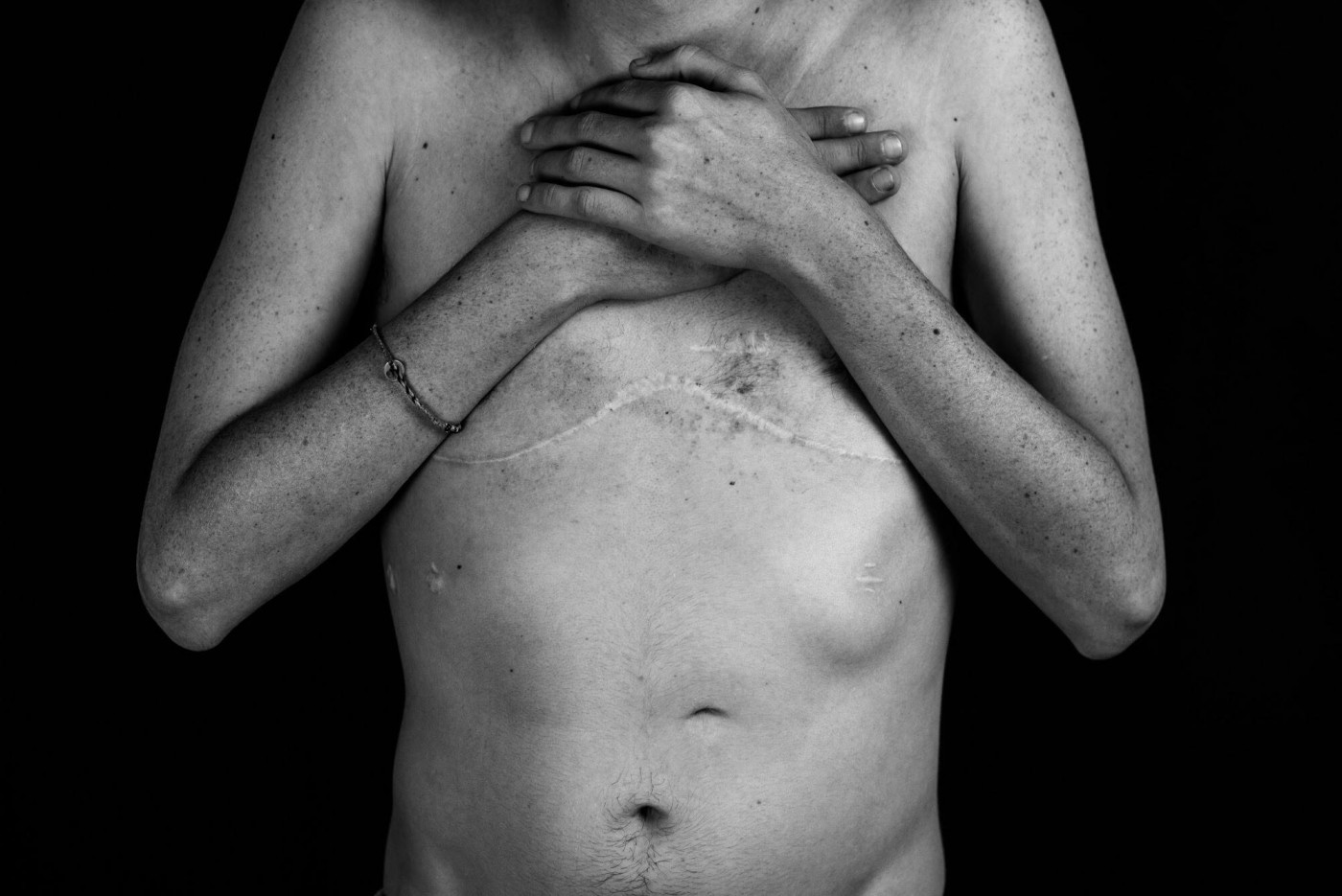
My body bears the marks of my traumatization. (Photo by Kathleen Sheffer)

I walk through a football stadium. I catch a whiff of the cotton candy and am smacked back to every procedure I’ve had, breathing in the stale cotton candy-scented anesthetic before I drift to nothingness. I am so overcome with fear that I feel like dropping to my knees and letting the world swallow me.
I watch a movie about a child who becomes deaf. They scream on-screen in terror, and my heart screams with them as I remember losing my hearing to IV amikacin. I’m sweating so badly.
I can’t breathe, mucus plugs my lungs so thickly. The doctors are telling me my new transplanted lungs have CF, that they didn’t know my donor had it too. I wake up from the nightmare with a gasp, poke at my ribs, and don’t fall back to sleep.
A week ago, I met a post-heart transplant recipient and a lung transplant recipient with CF. The heart transplantee (she had a rare condition later in life) sighed about how much CF patients go through in their lives. The other CFer and I swapped a quick glance. She and I had spent the past four hours exchanging medical histories — which bugs were cultured, how difficult it is to gain weight, which difficulties we faced after transplant, stuff like that. We spoke of life pains casually; pains that once brought us tears and severe anxiety. And often still do.
We are adults now. We are thick-skinned and battle-hardened. But there was a time when we were children. One of the worst parts of CF is that it’s a childhood disease. Most patients suffer early on in life, long before they have a chance to build their emotional defenses. Many of us carry the traumas of CF childhood into adulthood, as much as we’d like to think it’s all behind us.
CF patients are two to three times more likely to have anxiety and depression compared to the general population. I was diagnosed with anxiety disorder and panic disorder in 2010, along with situational depression. Mental disorder is often depicted as a side effect of chronic disease — it’s “to be expected” for those who suffer. I think there’s truth to that, but it shouldn’t be treated any less seriously because of it. I’m angered when CF patients are told to “deal with it” because there are too many physical ailments to address. It’s a story I’ve heard over and over from my fibros and cysters.
CFers: Your emotional struggles can be as mighty as your disease. Don’t let anyone belittle those problems.
I’ve been digging through memories and life patterns to identify the roots of my mental discontent. I keep revisiting flashbacks of my septic shock and ICU psychosis of last summer — memories of being strapped to my hospital bed, of the hallucinations, of the blind fury I felt. Stacked upon those memories are vivid flashbacks of Little Brad’s experiences of being smashed against the grindstone of life.
I think of Little Brad as a completely different person. My heart aches when I think of him being hurt, cut and poked, but not understanding why. Of being on that cold, hard operating table surrounded by masked strangers without mommy or daddy. Of knowing his best friends are playing hide ‘n seek, while he’s hiding beneath hospital sheets from doctors.
The grindstone has made me stronger in many ways, yes, but the truth has finally clicked with me: I am traumatized.
I’ve previously acknowledged I experienced trauma in recent years and have devised strategies for healing place-based trauma. But I was in denial, thinking all trauma was either of the past or on its way out the door. Instead, it’s something I carry with me every day no matter where I am. I am traumatized by even my earliest memories of CF-related torment.
I’ve spent two decades avoiding that statement, “I am traumatized.” I wanted to tell everyone I’m brave and tough. For my parents’ comfort, for my friends’ respect, for my own sense of self-security. Now, I realize I am brave and tough because I am traumatized. I am a haunted survivor, but I’ve continued to fight through caustic antibiotics, every lethal infection, and transplantation to continue the relentless pursuit of my dreams. These dreams kick back at the nightmares.
The admission of continued trauma gives me power over it. The declaration introduces new opportunities for treatment and an evolved understanding of my psyche. My trauma might always be a part of my life, but it doesn’t need to have control over me. How can I free myself from its control? I don’t know yet, but I intend to.
To a CFer or loved one of a patient: I write this in hopes that you can come to grips with your past and present in dealing with this disease if you are traumatized. You can still be strong while acknowledging the horrific suffering CF has inflicted on your emotions.
***
Note: Cystic Fibrosis News Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Cystic Fibrosis News Today or its parent company, Bionews Services, and are intended to spark discussion about issues pertaining to cystic fibrosis.








david skeens
Im sorry your going through such a miserable time My son had CF not as lucky as you most of them kids also arnt as lucky as you I would give my left arm to be able to play and hug and talk to my little peanut for one more year let alone 20 he lived to be almost 4 always in the hospital bravest little guy I ever seen but we have something in common ive been traumatized also by Cf but I spread the word and never let his memory die I know how awful CF is but I wish he was here able to tell his story so lets burry the past because all those kids who died so young are depending on you to get up get out and help save these kids so they wont go through what you did or not go through anything except ICU doors maybe you can turn your trauma into how lucky you rally are we are all depending on you to get the word out to help cure this awful awful Cystic Fybrosis
Jen
As a fellow CFer and lung transplant patient, I want to thank you for this article and for your honesty. Anxiety and depression has been part of my experience throughout the years as well and there should be no shame in admitting it.
chad
As a parent of a 7 year old with CF, this is heartbreaking to read. I can't imagine what it's like to live through. I wish you the best in learning how to live with the challenges you have. Thanks for sharing your perspective.