Emerging Bacteria Species Shows Antibiotic Resistance, Patient Transmission
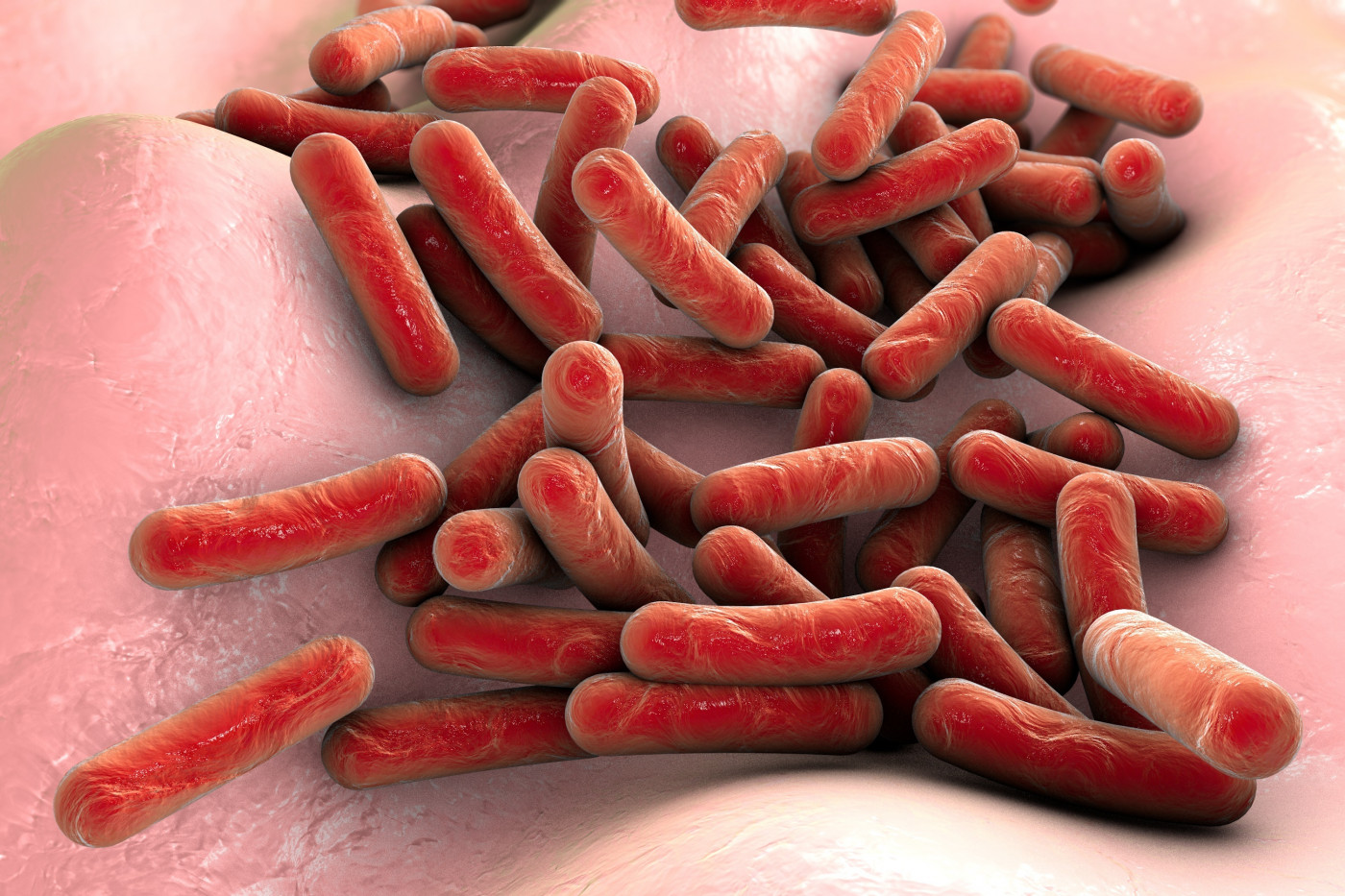
The Achromobacter bacteria species that is an increasing source of chronic lung infections in people with cystic fibrosis (CF) shows evidence of patient-to-patient transmission and emerging antibiotic resistance, scientists in Denmark report.
Their study, “Transmission and antibiotic resistance of Achromobacter in cystic fibrosis,” was published in the Journal of Clinical Microbiology.
Most CF live with chronic bacterial airway infections, due to problems with mucus production and clearance. The most common pathogen in these infections is Pseudomonas aeruginosa.
But recent studies are reporting the bacteria species Achromobacter is increasingly being detected in CF patients, and associated with antibiotic resistance and more severe disease.
Little is known about the transmission of this bacteria, however, and its antibiotic resistance among patients.
A team led by researchers at the Center for Genomic Medicine in Copenhagen conducted DNA analysis on Achromobacter bacteria isolated from 51 CF patients. Their goal was to further understand how these pathogens spread and how resistant they are to treatment, which is needed to effectively manage and eliminate this pathogen.
All patients received early antibiotic treatment for Achromobacter after first testing positive, with follow-up treatments based on antibiotic susceptibility testing to find the most effective therapy.
In total, 182 genomes were analyzed from 101 clinical isolates of Achromobacter from the 51 patients. Of these people, 32 (63%) were chronically infected with Achromobacter, meaning half or more of their samples tested positive for Achromobacter over a year.
Before this study, all isolates included were identified specifically as the Achromobacter xylosoxidans using routine microbiology techniques.
But following DNA analysis, the researchers found their collection was composed of five different Achromobacter species. These included 15 (25%) patients infected with A. ruhlandii, 12 (20%) with A. insuavis, 31 (52%) with A. xylosoxidans, and one with A. aegrifacies. Another patient was infected with a yet unknown Achromobacter species.
To investigate patient-to-patient transmission, genome results were compared to identify specific bacteria with a related common ancestor (same clonal type), which was defined as bacteria that differ by less than 5,000 single-nucleotide variants (SNV) — single changes in the building blocks of DNA.
More closely related bacteria within a species, which suggests close transmission, will have less genetic variation than more distantly related bacteria within the same species. The analysis found 16 suspected patient-to-patient transmission cases that were investigated further.
In 12 of these cases, multiple clonal relatives were isolated from at least one of two patient pairs, and in nine of these cases, isolates from different patients were more closely related than those from the same patient.
Next, a phylogenetic tree (similar to a family tree) was constructed based on the genetic relationship of the four suspected patient-to-patient transmitted clonal types — one clonal type of the A. ruhlandii species, one A. insuavis, and two from the A. xylosoxidans species.
Of 14 suspected transmission cases with full phylogenetic information, 12 cases supported patient-to-patient transmission as bacteria from one patient was found to be descended from bacteria from another patient.
To support this genetic evidence of transmission, researchers looked for overlap in patient visits to the clinic. Of the 16 patient pairs with suspected transmission events, all but one patient pair with microbial sampling were in the same hospital ward on the same day.
“[S]uspected transmissions tended to happen in patients with more contact days than non-transmission patients,” the team wrote.
Overall, 15 out of 16 suspected patient-to-patient transmission cases were supported by genetic analysis, and phylogenetic or epidemiological data. The A. ruhlandii clone type AX01DK01 showed the most transmissions, being found in 27 isolates across 13 patients.
These bacteria were previously shown to be hypermutable, meaning abnormally frequent DNA mutations. A similar hypermutable state was identified in A. ruhlandii AX01DK01 from this study. Further analysis also identified two other clonal types as hypermutable, A. insuavis AX02DK06 and A. xylosoxidans AX03DK11.
“[W]e noted that hypermutable clone types were exclusively found in patients clinically defined as chronically infected,” the researchers wrote.
To investigate antibiotic resistance, routine diagnostic measurements of antibiotic susceptibility profiles were assessed against 21 antibiotics for 92 isolates. For the 21 patients with single isolated samples, these bacteria were resistant or intermediately resistant to a median of 14 antibiotics. For 30 patients with multiple samples over time, those isolated early were resistant to a median of 14 antibiotics, while those collected later were resistant to 18 antibiotics.
Statistical analysis found bacteria isolated later to be significantly less susceptible to antibiotics (meaning more resistant to them) than early and single isolates. Nearly all isolates showed resistance or intermediate resistance to nine antibiotics; five showed some efficacy. No antibiotic was effective against all the bacteria tested.
Compared to other Achromobacter isolates, A. ruhlandii AX01DK01 bacteria were resistant to a median of 20 antibiotics. Furthermore, seven out of 29 A. ruhlandii isolates were resistant to 21 antibiotics, while only one A. insuavis isolate and none of the A. xylosoxidans isolates were resistant.
“[We] found genomic and epidemiological support for suspected patient-to-patient transmission in all three Achromobacter species and suggest a new measure — gene content difference — to be taken into account when evaluating suspected between-patient transmission cases,” the researchers wrote.
“Finally, we showed that antibiotic resistance develops in all three Achromobacter species.”
These results, the team added, “allow us to better understand antibiotic resistance dynamics and patient-to-patient transmission of Achromobacter in patients with CF which could help predict clinical progression of Achromobacter infections and prevent patient-to-patient transmission.”







