CF Foundation Supports Work on Antifungal Therapy for Lung Transplants
The Cystic Fibrosis Foundation announced a $3.5 million investment in Pulmocide to support the company in developing an inhaled medication, opelconazole, to prevent fungal infections — specifically Aspergillus — in lung transplant patients.
This funding will go toward a planned, multicenter Phase 2 clinical trial of opelconazole to assess the therapy’s safety and tolerability. It will also evaluate transplant recipients’ ability to complete a course of the treatment in preventing fungal lung infections, and opelconazole’s degree of drug-drug interactions with other medications.
This funding marks the foundation’s first support of work on a therapy specifically for lung transplant recipients.
“We are hopeful not only that this potential treatment could help prevent lung transplant recipients from getting a devastating Aspergillus infection, but also that if successful, it could eventually help all people with CF who have chronic Aspergillus infections,” Albert Faro, MD, the CF Foundation’s vice president of clinical affairs, said in a press release.
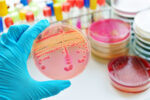
Aspergillus is the most common cause of fungal infections following lung transplant. Those with cystic fibrosis (CF) are at particular risk of Aspergillus infection post-transplant due to the potential presence of the fungus in their airways prior to the procedure.
Current treatment options for people infected with Aspergillus can be difficult to tolerate, leading to patients discontinuing the treatment before completing the full course. Some treatments may also interact with other transplant medications, potentially causing serious side effects, the foundation noted.
Opelconazole is a new triazole antifungal agent that works by targeting a pathway used by fungi to create a component of their cellular membrane. As such, it aims to disrupt fungal membrane structure and prevent further growth.
It is designed to be inhaled to maximize the amount of antifungal medication that gets into the lungs and to limit bodywide effects, potentially preventing drug-drug interactions. Inhalation can also allow for the medication to be administered at the home.
Opelconazole has been well-tolerated with “remarkable” clinical responses to its use under a Special Needs program at several clinics across the U.K., Pulmocide reported in a separate press release. A variety of patients who “failed previous antifungal treatment options responded well when opelconazole was added to their treatment regimen,” it stated.
The foundation’s support comes through its Lung Transplant Initiative — part of its commitment to support CF patients throughout their journey — established in 2016. The nonprofit notes that historically about 200 people with CF undergo a double-lung transplant each year, and that post-transplant outcomes can vary widely in this patient group.
“The CF Foundation’s support to further the development of opelconazole as a vital option for the prevention or treatment of pulmonary aspergillosis in people living with cystic fibrosis who have received a lung transplant is greatly appreciated,” said Lance Berman, MD, chief medical officer of Pulmocide, which is based in London.
According to the company, opelconazole has the potential to be used in a variety of lung conditions in which Aspergillus has been implicated, including chronic pulmonary aspergillosis, severe asthma, allergic bronchopulmonary aspergillosis, chronic pulmonary obstructive disease, severe flu, and lung damage subsequent to COVID-19.