Every March, My Body Remembers the Trauma of Almost Dying

March is a heavy month. Like clockwork, physical and emotional symptoms seem to erupt out of nowhere. Four years ago this month I almost died. On an unconscious level, our bodies remember the trauma we’ve endured.
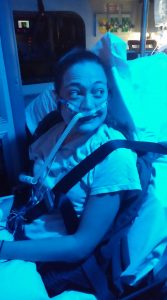
March 2017 was the most difficult month of my life. I’ve never fought harder to stay alive. I went into respiratory failure and was moved from the regular floor at my local hospital to the intensive care unit. It was terrifying to be in the ICU for the first time.
I was on the maximum flow of oxygen (60 liters per minute) because I was oxygen deprived and air hungry. I was unable to walk more than 5 feet without pausing to catch my breath.
Even with high-flow oxygen, I was desaturating. My level of functioning was plummeting quickly. I couldn’t perform basic personal care tasks independently.
My lung transplant team in Boston collaborated with my local Vermont CF team. Thank God my transplant evaluation had been completed the previous August. But my six-minute walk test had expired and Boston required me to be transported there to do it.
Afterward, I was immediately listed for a double-lung transplant. Sicker than ever before, I was placed at the top of the transplant list.
A medication side effect caused fevers during this time. The morning after being listed, I woke up breathless on the maximum amount of supplemental oxygen. The doctors filtered in and out of my room that day devising a plan to intubate me and connect me to an ECMO machine. As soon as they left the room to activate their plan, I turned to my mom, who was at my side, and whispered, “It’s time to rally.”
I can’t explain the supernatural force that strengthened me that day, but God definitely took over the situation. I got the medication I needed to reduce the fever. Miraculously, within a few hours, my fever had vanished, I could breathe well enough to talk again, and the doctor’s plan was canceled.
The pain of being in respiratory failure and dying is difficult to describe. Every part of me hurt, and this was magnified by how every breath felt like a marathon. Not to mention the mental, emotional, and spiritual toll it took on me. It was the closest to death I’ve ever been, and I felt it on every possible level.
Five months later, I received new lungs. This August will mark four years of breathing in a whole new way. While the transplant saved my life, the trauma left residual side effects I wasn’t prepared for.
In “The Body Keeps the Score,” author Bessel Van Der Kolk, MD, explains the mind-body connection. He details how our bodies remember every traumatic event we’ve experienced on both physical and emotional levels. Our cells retain the information from those memories and store them as part of our cellular makeup.
My first March post-transplant, I went to the emergency room with chest pressure, horrible headaches, and shortness of breath. I thought I was having repeat blood clots.
Doctors ran multiple tests and confirmed nothing was wrong with me. This happened a few times that month. I was also extremely anxious and severely depressed. Nothing had precipitated the onset of these symptoms.
I started seeing a trauma therapist around this time. He taught me that the body holds on to traumatic memories, and that they can express themselves as physical and emotional symptoms. This was eye-opening, relieving, and reassuring, and it completely made sense considering the trauma I’d endured. There was a reason I was feeling like this. I wasn’t crazy.
My therapist also confirmed that there was no new tissue damage happening in my body. My body was reliving the physical sensations I had experienced the previous year.
This has happened every March for four years. Each year has gotten a bit easier. I’m not surprised anymore. Rather than dreading this month, this year I forgot! It took me a few days before I remembered what month it was and where the symptoms were coming from. There was a hint of panic, then relief that I was OK, at least in the sense that nothing new was wrong.
I’ve developed coping strategies for supporting my body and mental health through this month. I loosen expectations for my productivity and energy levels. I give myself permission to rest more, introvert hard, and reach out for support.
When we open our hearts for encouragement from those who have waged the same war, it comforts us in a security-blanket kind of way. We are not alone.
***
Note: Cystic Fibrosis News Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Cystic Fibrosis News Today, or its parent company, Bionews, and are intended to spark discussion about issues pertaining to cystic fibrosis.









April Biggs
Lara - great piece. I appreciate taking a moment to acknowledge how trauma lives on in the body. I'm in the process of writing my memoir and this is something I keep processing. Happy we're both still here.
From a disability perspective, I advocate for all of us to do this on the regular: "I loosen expectations for my productivity and energy levels. I give myself permission to rest more, introvert hard, and reach out for support."
Lara Govendo
Dearest April, thank you SO much. I know you feel this deeply. So grateful we are both still here to tell our stories. And I'm excited to read your memoir! Yes, amen sister. Love the important work that you're doing xoxo