Enduring the nightmare of COVID-19 as a transplant recipient
For this CF patient and transplant recipient, COVID-19 caused deep anxiety
Written by |

After I had flown under the radar for three years to avoid it, COVID-19 eventually hit me like a ton of bricks last January. Having cystic fibrosis (CF) and transplanted lungs added to the fear of what this virus might do to me.
It started on a Thursday night. My eyelids were heavy with exhaustion. It was the end of my work week, and I thought I just needed a good night’s sleep to catch up. Working as a therapist for kids is depleting, so I didn’t think it was out of the ordinary.
But I couldn’t get warm. Again, I thought it was normal because I live in Vermont, and late January brings average temperatures of below freezing. I piled on the extra blankets and fell asleep. In the middle of the night, I woke up to pee and felt like I was burning up. “Must be too many blankets,” I thought. I touched my head and belly, and both were on fire. I quickly checked my temperature and my heart sank. The thermometer read 103.5 F.
I contacted my transplant team (at a reasonable hour). They requested that I be examined locally and get a respiratory panel. I got an appointment with the on-call doctor at the weekend clinic. (Why do these things always happen on the weekend?)
I religiously checked my email for results from the viral swab. Rolling in at 11 p.m., the final results declared that I was positive for COVID-19.
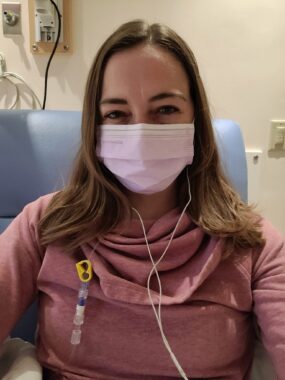
Lara receives a boost from an intravenous infusion of fluids with electrolytes. (Photo by Lara Govendo)
Steeped in medical trauma
The floodgates opened and the tears flowed with a vengeance. I’d spent the last three years protecting my new lungs from this scary, unpredictable virus. I wore a mask around everyone and sanitized everything I touched, but the virus managed to jump through the barricade I had built around myself.
My immediate thoughts circled around death, naturally. My mind tends to wander there as a result of residual trauma after several near-death experiences. I have friends who died of COVID-19, and I had no idea how my body would react. Also, I’m not vaccinated because of my history of blood clots, but that’s another story.
My transplant team said that there wasn’t anything they could do for me. A pre-exposure prophylaxis antibody infusion isn’t effective against most COVID-19 variants anymore. An antiviral pill would have required that I stop taking antirejection medication, so that wasn’t an option, either.
COVID-19 caused traumatic memories of life with CF lungs to resurface. I experienced the same heightened anxiety while trying to sleep because my breathing had changed. I’d jolt awake with a feeling that I couldn’t breathe and anxiety that I would suddenly stop breathing. I also had a deep, productive cough with shortness of breath, which added to reliving past traumatic events.
COVID-19 also impacted my immune and digestive systems. It wiped out my blood counts, knocked my heart rate down to the 50s, and caused my blood pressure to tank. My body fought hard, then was completely depleted because it doesn’t replenish easily like typical immune systems do. I lost my appetite and was extremely nauseous, which prevented me from filling my depleted body with the nutrients it needed.
I whipped out the arsenal of healing methods that had worked for me prior to my transplant. I used natural remedies to clear my lungs, nebulized to keep my airways open, used sinus rinses, drank tea, swallowed vitamins, and forcefully ate homemade chicken soup. And thankfully, after going for acupuncture and getting a few infusions of fluids with electrolytes, I bounced back to functioning.

There’s nothing better than an ice-cold ginger ale to beat nausea. It’s a fan favorite at the hospital. (Photo by Lara Govendo)
I incorporated ways to feed my mind and spirit daily. Going for walks kept my lungs and mind strong. I listened to uplifting music and podcasts, watched funny movies, and talked to loved ones to stay connected.
Even though I live alone, loved ones helped me. Family and friends prayed with me and texted me encouragement. Dear friends dropped off homemade chicken soup and groceries at my door.
If anything, catching COVID-19 reminded me that I still know how to fight for my life. It’s been a luxury to be healthy lung-wise, but how soon I forget that the body really does keep the score.
Note: Cystic Fibrosis News Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Cystic Fibrosis News Today or its parent company, Bionews, and are intended to spark discussion about issues pertaining to cystic fibrosis.








Leave a comment
Fill in the required fields to post. Your email address will not be published.